Researchers develop new technique to unveil ‘matrix’ inside tissues and tumours
Scientists from the Biotech Research & Innovation Centre (BRIC) at the University of Copenhagen have developed a groundbreaking method to reveal the structure of tissues and tumours with unprecedented detail, by completely dissolving away cells and leaving the delicate extracellular matrix intact.
The matrix surrounds the cells in every organ of our bodies, and provides shape and structure to the organ. The matrix has a profound impact on how cells behave, and so controls the progression of diseases such as cancer. Yet the matrix is extremely difficult to study in detail.
Now a team of researchers led by Professor Janine Erler has developed a new technique just published in Nature Medicine that makes closer study of the matrix possible. The technique reveals the inner structure of organs and tumours by removing cells but leaving the matrix completely unaltered. The three-dimensional structure of this matrix has never been seen in such detail before.
“We have developed a technique to obtain intact organ scaffolds and to image them in incredibly high detail using microscopes. We are the first to image the 3D structures of primary and metastatic tumours as well as healthy organs in this way”, says Professor Erler.
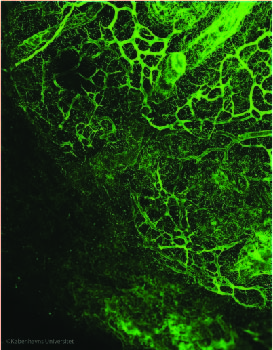
The extracellular matrix structure revealed. A de-cellularised cancer growth. Image by Alejandro Mayorca-Guiliani.
A world of details revealed
Cells which are organised together to form tissues rely on the extracellular matrix as a foundation for attachment, to arrange themselves properly, and to sense how to behave when their environment changes. Sometimes this organisation goes wrong and cells grow into tumours. To destroy a tumour, it is essential to know both its structure and the foundation upon which it is built.
The new method was pioneered by postdoctoral fellow Dr Alejandro Mayorca-Guiliani, in Professor Erler’s team, who says, “We have isolated the structure that keeps tissues in place and organises the cells inside them. We did this by using existing blood vessels to deliver cell-removing compounds directly to a specific tissue to remove all cells within an organ. Doing this leaves behind an intact scaffold that could be analysed biochemically and microscopically, providing us with the first view of the structure of tumours.”
Imaging expert and co-first author Chris Madsen (now at Lund University, Sweden) says “When you remove the cells, the clarity of what you can see through the microscope is much improved – you can see the fibres of the matrix more clearly and you can look much deeper into the tissue. Using this approach, we have been able to see important differences in matrix organisation when we looked at metastatic tumours in the lung and in the lymph node.”
Matrix biology and mass spectrometry expert and also co-first author Thomas Cox (now based at the Garvan Institute of Medical Research, Australia) says “Because we are removing the cells completely, we can use mass spectrometry to identify and catalogue the components of the matrix – in normal tissue and in tumours – in unprecedented detail. What is really exciting is we found that some of the components of the matrix in different secondary tumours [metastases] are unique to that tissue. That is telling us that remodelling of the matrix in cancer is organ-specific”.
Understanding cancer progression
This research is an advance in the fields of both cancer research and bioengineering: By using the decellularised organs we can learn much more about how tumours and normal organs are built, and what their differences are. This new technique might even have an impact on organ regeneration and tissue engineering in the future.
“We are now re-introducing cells into our extracellular matrix scaffolds, bringing them back to life, to study how tumours form and how cancer progresses. This is extremely exciting and offers a unique opportunity to study how cells behave in their native environment,” explains Professor Erler.
The research is supported by the Danish Cancer Society, a European Research Council Consolidator Award, the Novo Nordisk Foundation, the Ragnar Söderberg Foundation Sweden, Cancerfonden Sweden, the Innovation Foundation Denmark, the National Health and Medical Research Council (NHMRC) Australia and the Danish Council for Independent Research.
For more information, contact:
Professor Janine Erler, BRIC, Janine.erler@bric.ku.dk
Lonnie Moldt Jørgensen, Communications Officer, BRIC, lonnie.jorgensen@bric.ku.dk
Contact
Professor Janine Erler
Email: Janine.erler@bric.ku.dk
+45 35325786
Lonnie Moldt Jørgensen, Communications Officer
Email: lonnie.jorgensen@bric.ku.dk
Original article
'ISDoT: in situ decellularization of tissues for high-resolution imaging and proteomic analysis of native extracellular matrix'. Nature Medicine (2017). DOI: 10.1038/nm.4352.
